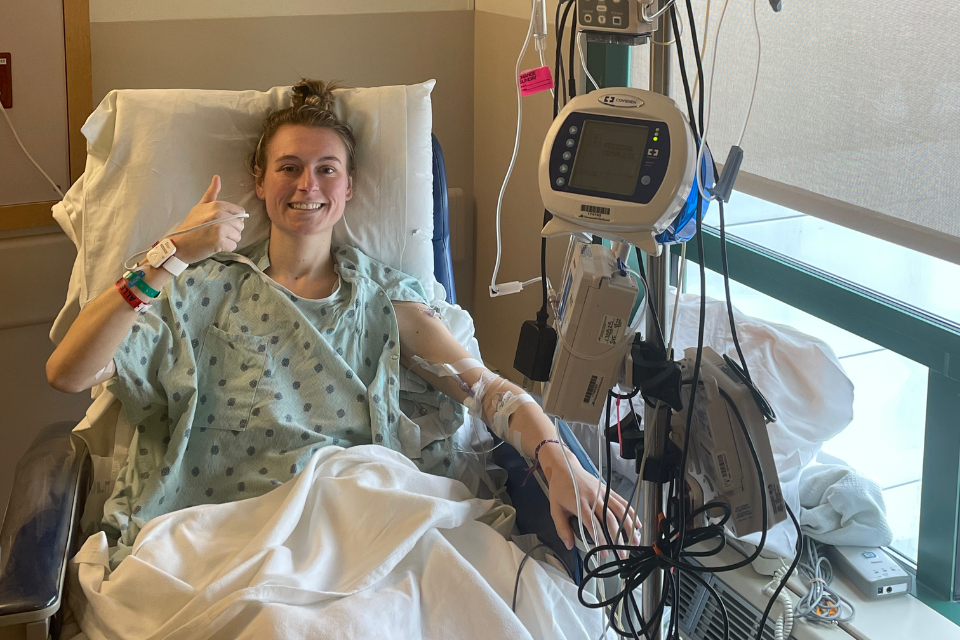
Interview with Chronic Pancreatitis Patient, Christine Cataldo
In the summer of 2018, Mission: Cure’s intern, Gabriela Gil, sat down with Christine Cataldo, a patient volunteer with Mission: Cure, to learn more about Christine’s experiences living with chronic pancreatitis. Diagnosed with pancreatitis linked to the PRSS1 genetic mutation in 2002, Christine shared stories how her condition was identified, discussed her family’s relationship with the disease, and emphasized the importance of patient advocacy in pancreatitis research:
Question: Can you tell us a little bit about yourself?
Answer: The biggest things in my life are my three girls, all five and under. They take up most of my time, but I also work part-time as a tax consultant on international issues for PwC, which has luckily given me the flexibility to reduce my schedule ever since I had my first daughter. Outside of that, I spend time with friends and family. I also spend time being active, and I strive to prepare healthy meals for me and my family. Exercise is a stress outlet, a personal interest, and a way to spend time with my kids. Health in general has always been an interest of mine, and now, due to pancreatitis, it is a must to manage the disease. In the summer, I like to go to the beach; I live in a small coastal town in Connecticut and I grew up in Virginia Beach. Oh, and I am a huge Washington Redskins fan, which is a little unique for someone living where I do.
Question: When were you first diagnosed with pancreatitis?
Answer: I was first diagnosed in college. There was a string of events that led to my diagnosis. I was lucky in a way (to be diagnosed) because I had always experienced episodes of acute pancreatitis, but I had never realized that was what it was. I didn’t realize that it wasn’t the normal stomach bug. I didn’t realize that most people don’t regularly get really bad stomach bugs that are extremely painful.
On Thanksgiving break during my fourth year of college in 2005, my cousin was sick and curled up on her bed. She actually knew that she had pancreatitis because her sister (my other cousin) had been diagnosed with it when she was younger than 5. While I knew her sister was very sick as a child, I didn’t know it was because of pancreatitis, and I never thought I had the same disease as her because I wasn’t nearly as sick as a child. However, when I saw her having an attack this time, I knew that whatever she had, I had too. The next time I had a flare, in 2006, I went to the ER at UVA and told them I had pancreatitis. Of course, they didn’t believe me because I was so young, and I had diagnosed myself. Not only was my age atypical, but they told me that the typical individual with pancreatitis would be a man in his 60’s with a history of alcohol abuse. Even though this is incorrect, it misled them because clearly I was none of those things.
I was in the hospital for about four days, and they ran a genetic panel, that included cystic fibrosis and other known mutations. As I was checking out of the hospital, they informed me that the test results showed that I have hereditary pancreatitis (PRSS1 gene mutation). They didn’t explain to me that recurrent acute pancreatitis can easily turn into chronic pancreatitis. They didn’t explain to me that pancreatitis leads to a higher risk for pancreatic cancer. In hindsight, it seems that they were more interested in determining why a young person had pancreatitis, instead of explaining what that meant for me and my life. To me, it wasn’t groundbreaking news that it was hereditary. I already knew pancreatitis it was hereditary because I knew my cousins had it. I didn’t know hereditary pancreatitis was rare, untreatable, or that it could be so incredibly life-changing. I thought I would have to manage my lifestyle to avoid getting acute pancreatitis. I just didn’t know…
Moreover, I didn’t think a lot about the significance behind my PRSS1 gene mutation until about 10 years later when my cousin’s daughter had GI symptoms and her mother contacted me. She wanted the information on the genetic testing I had done, so her husband (my cousin) could get tested. She asked if I could get my UVA medical records to identify my specific gene mutation because it’s much cheaper to test for a single mutation than to run an entire panel of mutations.
Question: How did you first realize that your chronic pancreatitis was linked to genetics?
Answer: The first time I was diagnosed with pancreatitis I learned that I had the PRSS1 gene. I know that is quite a rare situation, and I consider myself lucky to have both a diagnoses and a cause. While UVA didn’t ask for my consent for the genetic testing, it has saved me a lot of time and money looking for a cause. While I knew my cousins had pancreatitis, I didn’t know there was a specific associated gene mutation. Had I not been at a top-rated, research hospital, I am not sure how I would have found out and how long that would have taken. It is hard enough to convince a doctor you have pancreatitis let alone a super rare genetic mutation.
I began to focus on the mutation this past year and a half. Before that, I just led my daily life, but when I started to have daily pain, I began doing a lot of research on the disease and the mutation and got on Facebook to try to find other patients with the mutation. While my own life is impacted and is stressful, the main way the mutation has changed my outlook on chronic pancreatitis is regarding the impact it can have on my children. I want the disease to be treatable for the next generation. I’ve had two out of three of my daughters tested. One has the mutation, the other doesn’t. My third daughter is too young to be tested.
It is nice to know about the mutation in a way because I know what is causing the pain. It can be very difficult to be diagnosed with such vague symptoms. In my experience the average doctor is unlikely to come up with chronic pancreatitis as a suspect and even more unlikely to know the proper tests to diagnose it. Even throughout my pregnancy, I told my OB and nurses and a GI doctor that I had upper (abdominal) pain and that I have hereditary pancreatitis, but none of my doctors truly believed me that it was the source of the pain. I understand the doctors’ confusion because I have seen on Facebook how different everyone’s disease has progressed. You read these studies online, and it seems like there is this very typical development, but from my experience and talking to other people, it is clearly not that straightforward.
In my family, only my sister, who also has the PRSS1 mutation, and my kids have been tested. To my knowledge, my cousins have never been tested, but I’m pretty sure they have the mutation. My cousin who was impacted the most severely had her pancreas removed before the PRSS1 mutation was identified. My mother has never been tested, but I think she probably has it because two of her kids have it. My brother was thinking about getting himself and his kids tested, but none of them have any symptoms, at least so far. In a way, it is scary to know.
My genetic counselor and pediatrician recommended not to get my kids tested until they presented symptoms, but I just had to know. I had to know. I might hold off testing my third daughter because it feels like coming to terms with a pre-written future and now I understand my doctor’s recommendation. You only focus on this one detail. It’s good to know of the mutation if you have pain and symptoms because you know the cause, but there’s nothing currently known to alter the outcome. The only other benefit to knowing about the mutation is that there is a higher risk of pancreatic cancer, but there are not currently any early diagnostic tools to easily detect pancreatic cancer, and treatments have only helped the minority of patients. The reason why I got my kids tested hasn’t changed – I had to know, but there is no denying that it is scary. It is what motivated me to get involved with Mission: Cure.
The last thing I will say is if you have been diagnosed with recurrent acute pancreatitis, have pancreatitis at a young age or have been diagnosed with chronic pancreatitis – fight, fight, fight to be tested for the known genetic mutations. I would not assume that just because no one in your family has had symptoms that there is not a genetic link. First, my mother has no symptoms and I didn’t know of any family members that had symptoms nor did I know what the symptoms are. Second, medical problems of your extended family may not be shared or known and pancreatitis is a complex disease and presents very differently in each person – even for people with the exact same mutation. I would also say that the earlier that one knows of the identified mutation, the more active you can be to help fight for a cure while you are not battling a chronic disease. Any family with a genetic mutation will have to deal with this disease for every generation until there is a cure.
Question: What is one thing you wish physicians knew?
Answer: Only one? [laughs]
Besides a cure, I wish they had a better understanding of the lifestyle implications this diagnosis brings. I frequently feel at a loss deciding things like what to eat for breakfast because there is such a disconnect between the world of nutrition and the doctors. My intuition tells me there has to be a connection, and there are definitely other factors, but lifestyle must play a role. But exactly how?
In my family, it seems like pancreatitis is getting worse in each generation. My great grandmother, who I think the mutation came from, died in her late 80s. However, doctors have told me to take my pancreas out early before I die from pancreatic cancer. If I look back, my family history doesn’t reflect that, so there has to be something else at play. I wish they could tell me more than “don’t drink; don’t eat fat.” There has to be more…
I’ve had to explain what pancreatitis is to basically every physician -my OB, GI, Primary Care and Urgent Care- until I finally found a doctor I was happy with. My current doctor is the only doctor that I’ve interacted with who knew about hereditary pancreatitis, other than the doctor that initially diagnosed me. Throughout my pregnancy, I had chronic pain, and they just kept checking my lipase and amylase, which stops being raised when you aren’t having an acute attack or your pancreas is severely damaged. I think they thought I was exaggerating the pain.
Right now I have daily pain that ranges in intensity. Sometimes it goes away completely during the day or just for two minutes at night. Sometimes it’s a pain level of 6 or 7, but I’m not taking any pain medications. I have recently been experimenting with a extremely low-fat, gluten and dairy free diet, and I don’t drink alcohol. However, when I told one GI that I had these intermittent symptoms of upper GI pain and that I had pancreatitis, they asked if I was sure it wasn’t heartburn. I know it wasn’t heartburn. The pain is very different. I get heartburn, and this isn’t it. They finally sent me to get an MRI with contrast and some blood work, but the blood work they ordered wouldn’t have identified anything relevant. The results were normal, my liver function panel was all fine, and lipase was low. The doctors said that low lipase was okay, but in reality low means that your pancreas isn’t functioning the way it should. I chose not to do the MRI with contrast because I was nursing. I am now glad I didn’t because my doctor at Hopkins sent me for a CT with contrast, not an MRI.
I am so thankful for my doctor at Johns Hopkins, but I don’t know if I could have even gotten an appointment with him had my sister and I not known that we have the PRSS1 mutation. That makes it very difficult for other people. Moreover, I don’t think my doctor knows anyone with the mutation that isn’t having serious problems. But I know that there are people with the mutation without serious symptoms because of my own family. I think there are a lot of doctors that know nothing about this disease or the genetic mutations. There is a group of doctors that only see the very sickest patients, but there is also a group of patients that aren’t understood or seen by either group.
Question: What is one thing you wish other patients knew about living with pancreatitis?
Answer: I wish that patients knew what their diagnosis is because pancreatitis really does present a range of symptoms, but it seems that only specific types of patients get through the process of being accurately diagnosed. I wish that patients would all get genetically tested. If they knew the cause, it would provide some peace of mind and a course of action. When you are have flares, you know why. At least that is how I feel. And if patients have a mutation, I wish they would find out who else in their family does too. I also wish that patients could connect with other people that are suffering so that they know they aren’t the only ones. It can be less isolating. I wish they knew about more options other than total pancreatectomy. I don’t know what those options are, but…
Question: How have you gotten involved with Mission: Cure’s work?
Answer: I have spent countless hours researching pancreatitis and have come away fairly disappointed. Not that the medical research community doesn’t know a lot, but that a lot hasn’t been put into practice. I was looking for a way to get involved with an organization that I thought could improve the lives of patients and impact the course of the disease, either to cure it or to slow it down.
My husband knew my obsession with pancreatitis research and sent me an article that was posted on the blog of Mission: Cure. Intrigued, I looked to see who was operating the blog, and I emailed the address on the website asking if there was anything I could do to get involved. For other patients, I would recommend several ways they can get involved. First, I would spread the word to your patients and doctors about Mission: Cure. It is a new organization. Second, read about Mission: Cure and participate in any patient outreach. Third, don’t lose hope that a cure is possible. The doctors and medical researchers understand a lot about pancreatitis, and it is up to the patients to advocate for themselves to get more research and turn research into practical application.
Question: Is there anything else you would like to share with us?
Answer: I am really thankful for Mission: Cure. I know it is a very small organization, but I think it is going down the right path. I am motivated by their mission, and it gives me hope. Not so much for myself because at this stage, I might have to end up with a TPIAT, but this is the only avenue of hope that I’ve found for my kids and for other patients. And that is so important.
Share Your Story
Your story matters. If you’re living with pancreatitis or caring for someone who is, your experience can inspire and empower others who are going through the same thing. That’s why we want to hear from you! Share your story with us by clicking the button below.