Care Today
The Report
Over the course of 35+ interviews, we listened to stories of excruciating pain, anxiety, and hopelessness as individuals and their families grappled with the medical system in search of a diagnosis or even just sufficient care. These conversations highlight the immense impact of pancreatitis on the social, emotional, mental, and financial well-being of individuals and families – challenges that are rarely discussed while managing the physiological aspects of the condition.
Current Patient Experience
Limited understanding of pancreatitis results in delayed diagnosis or misdiagnosis of patients
Patients noted being misdiagnosed with conditions such as a sensitive stomach, gallbladder malfunctioning, irritable bowel syndrome (IBS), or appendicitis, or were told it was “in their head.” Several patients expressed frustration with providers failing to thoroughly investigate possible causes of their illness, and quickly brushing them off or sending them home when clinical tests or scans showed inconclusive results.
Outdated and inconsistent standards of care severely impact patients’ quality of life
Patients who did receive a diagnosis were often left on their own to understand and manage the condition. Several patients and caregivers reported feeling hopeless and extremely depressed when the diagnosis was followed by no explanation of the disease and no conversation around a treatment and/or management plan. They relied on fragmented online resources and support groups to get answers to their questions with minimal medical support.
Minimal support with managing pain adds to patient anxiety and reduces quality of life
Pancreatitis patients live with a fear of flare-ups— episodes of debilitating pain that can last one to three weeks—which leave them bedridden and incapacitated. However, patients are often afraid to ask for pain medication due to fears of being labeled as drug-seekers. Patients who were prescribed painkillers to manage pain were mostly given one or two options with no alternatives, even when the prescribed medicine was not a good fit for the pain or created other complications. Patients wished that their pain and suffering were acknowledged by their providers, rather than being disregarded and dismissed.
The disease’s impact on mental well-being is rarely discussed or addressed
The combination of the debilitating pain and lack of reliable information on pancreatitis can often be intimidating and isolating for patients who have just received the diagnosis and never heard of the condition. The excruciating pain combined with mental health issues often impaired patients’ abilities to fully engage in school, work, and other commitments.
The Patient Journey
What is the typical journey of a person living with pancreatitis as they navigate the medical system in search of a diagnosis and a care plan? In our report, we were able to map out the following patient journey.

A pancreatitis patient begins the journey by experiencing intense, excruciating abdominal pain.
They go to the ER; get some pain relief; may undergo some diagnostic tests; likely discharged with no clear diagnosis and/or referral to a GI.
They may make multiple visits to the gastroenterologist and/or other clinicians and undergo another set of scans and tests.
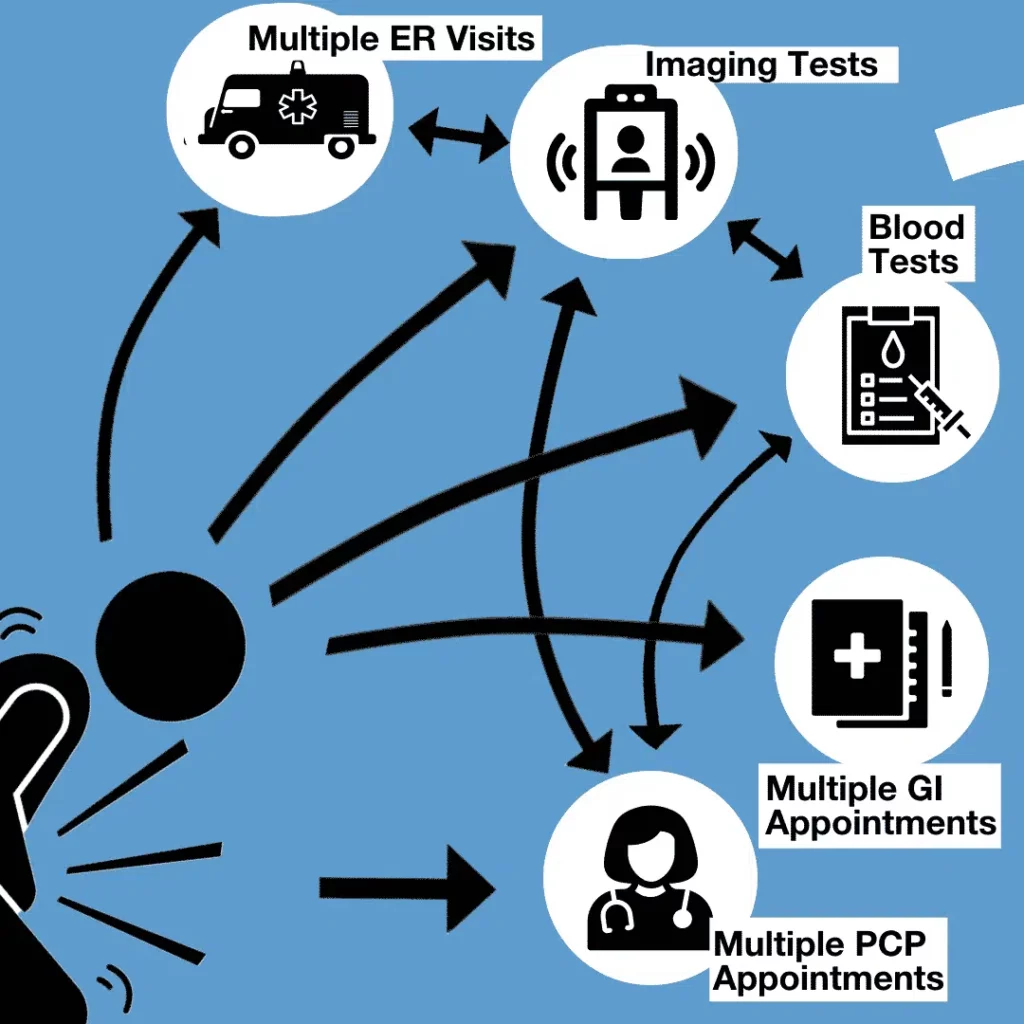
The person may end up making multiple visits to different GIs, urgent care and emergency departments, many times with no clear diagnosis or even a misdiagnosis.
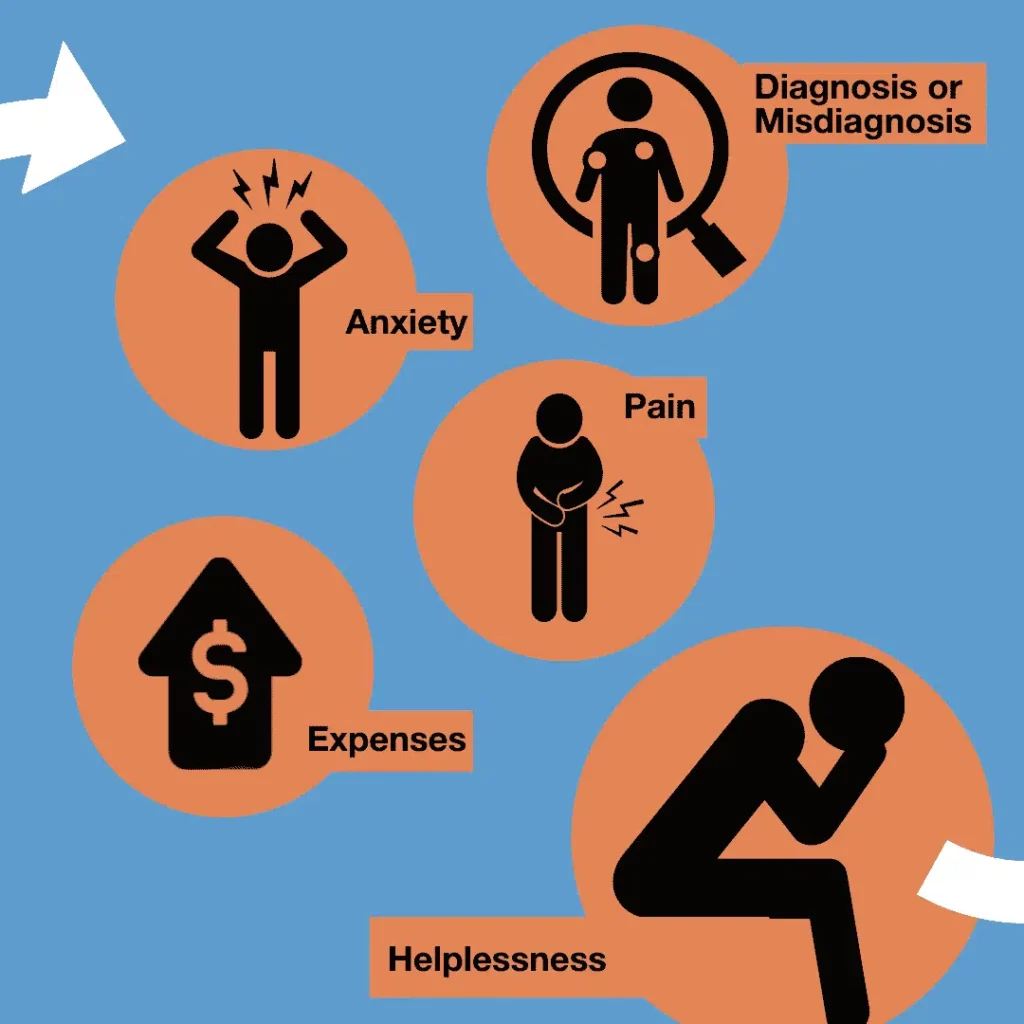
The person is left in a state of confusion, hopelessness, and anxiety while still managing pain.
Some patients who have the resources may traverse the country, seeking experts to diagnose their condition and/or create a plan to manage pancreatitis.
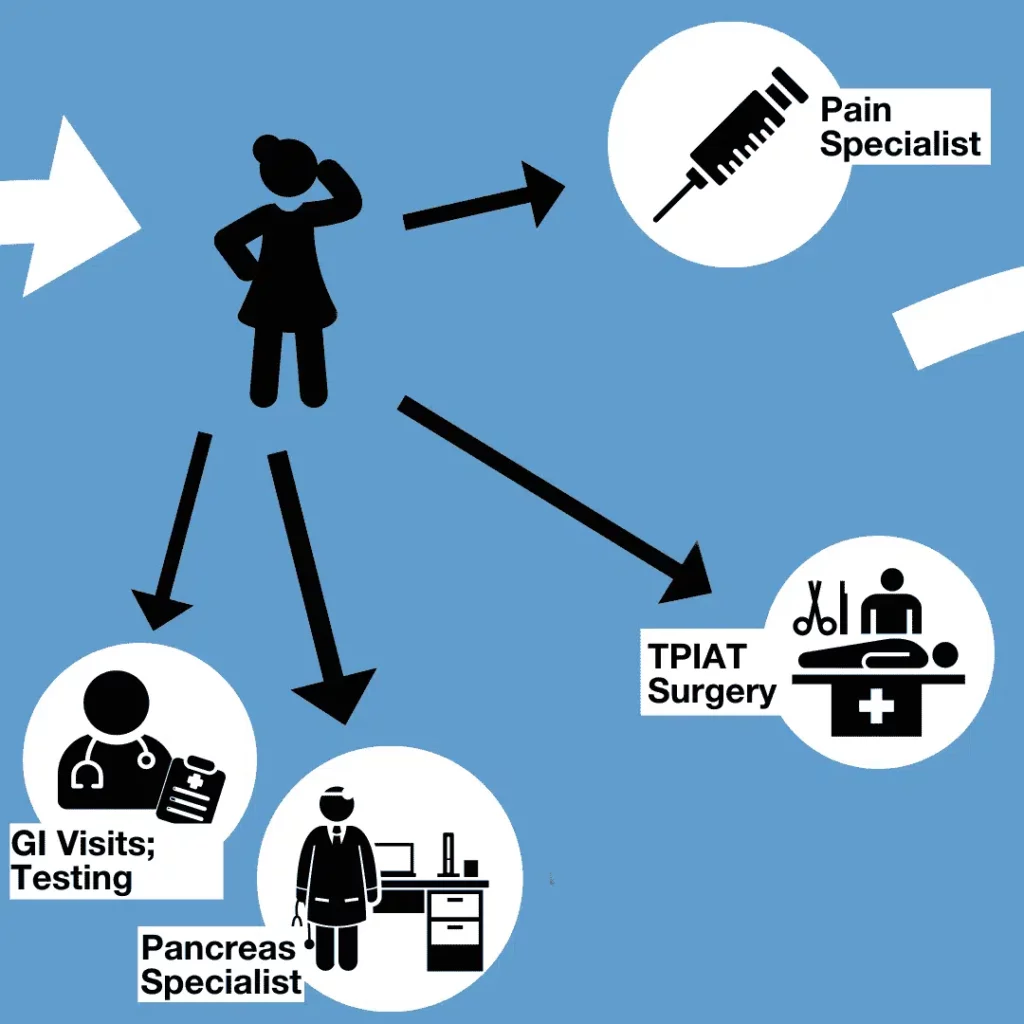
Armed with a diagnosis, the person may seek care from a trusted GI and pancreas expert.
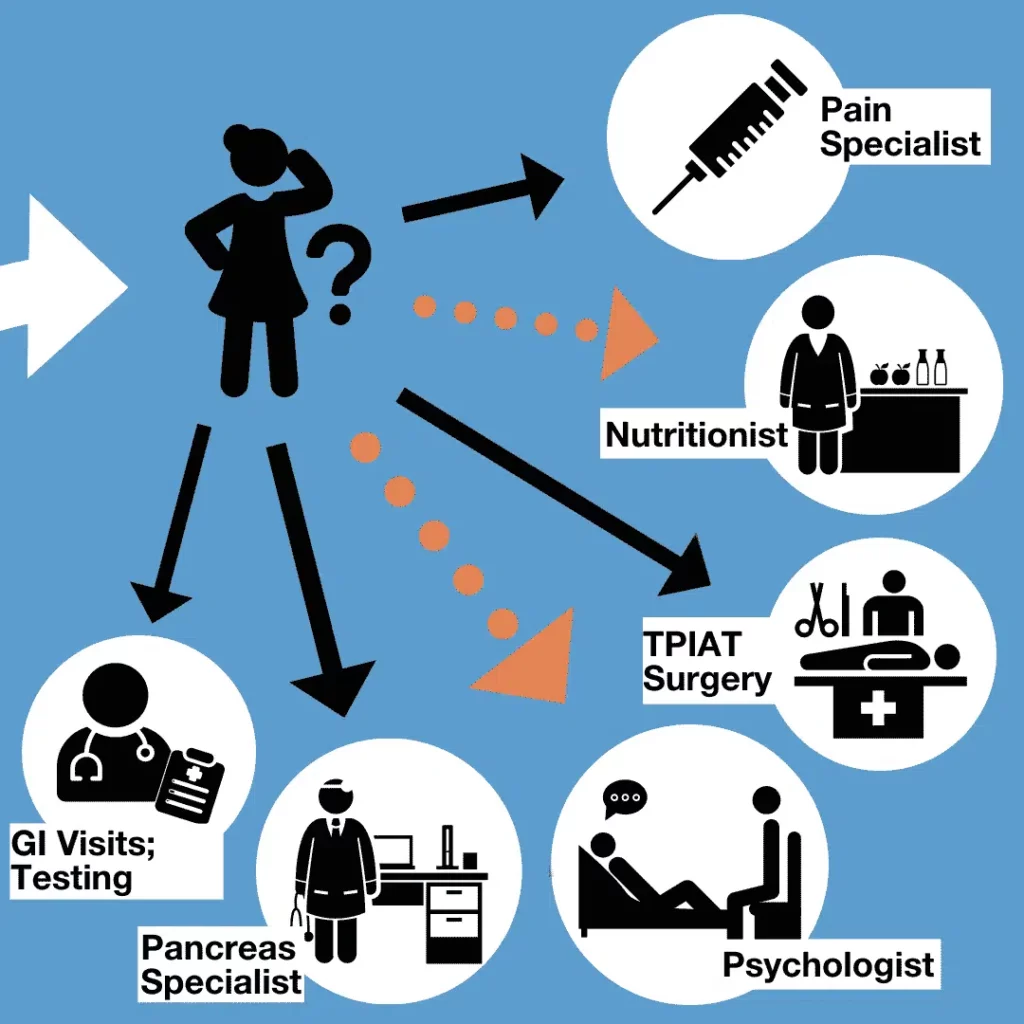
They may also seek help from other specialists to manage related complications. But in most cases, the burden remains with the patient (and/or the caregiver) to coordinate between different clinicians while carrying the burden of pancreatitis.
Patient Quotes
Pancreatitis patients face numerous barriers in accessing care. The following quotes are from pancreatitis patients, which bring their experiences to life.
Patient Priorities
Looking Forward: Reimagining Care
Pancreatitis patient priorities shared in this report shaped our framework, and we hope to spread and scale these practices so that all patients can access high-quality care when it comes to treating their condition.